
Curare is considered a poison in the world, although strictly speaking it is a very particular poison.
⚠️ The lethal effect of curare on human beings⚠️
Curare does not affect the blood circulation, the cardiovascular system, or the heart (see: types of poisons).

Curare acts as a neuromuscular blocker that ends up killing by asphyxiation. As if someone were entering the body to prevent breathing.
The neurotoxic venom, with which curare can be identified, produces flaccid and lethal paralysis by non-depolarizing neuromuscular blockade.
Respiratory failure is a side effect, resulting from cardiovascular shock or paralysis of the respiratory muscles.
Medical descriptions of a death caused by a high dose of curare refer to a person dying of asphyxia, without brain damage, with the heart beating, but no longer able to breathe, as if on an operating table where the dose of anesthesia had been administered incorrectly and the artificial respiration was not working.
✅ Acetylcholine
Acetylcholine is a chemical that facilitates the transmission of nerve impulses, and is found throughout the brain and in the autonomic nervous system.

Acetylcholine is a neurotransmitter, i.e. it mediates synaptic activity in the nervous system.
The nerve signal is transmitted through bioelectrical impulses generated by neurons and transported from one neuron to another, in the synaptic space, thanks to the action of neurotransmitters.
Neurotransmitters transmit signals from one neuron to another across the synapse, causing an excitatory or inhibitory effect on the neuron receiving the signal, i.e. the postsynaptic neuron.
Once acetylcholine acts, it is degraded by the action of an enzyme called acetylcholinosterase.
Acetylcholine is a substance of great importance in the autonomic nervous system, transmitting signals between motor nerves and muscles.
Thanks to the action of acetylcholine, muscle contraction occurs, since it mediates that muscle movement that has been stimulated by a nerve impulse.
Acetylcholine helps motor control, the voluntary movement of muscles, causing the contraction necessary for movement. If this signal does not occur, because acetylcholine is inhibited, the muscle does not move or muscle weakness and fatigue occur.
Where to buy acetylcholine?
Today acetylcholine is available in capsules as “brain food”.
It is said to improve cognitive function and alertness, help improve memory and improve the ability to focus on a mental task.
Curare binds to acetylcholine receptors and blocks it, preventing its action, producing muscular paralysis.
What are the effects of curare?
When curare reaches the blood it begins to act, producing motor muscle paralysis. The first muscles to be affected are the ocular and facial muscles.
Next comes the musculature of the limbs, neck and trunk. The intercostal muscles and diaphragm are then paralyzed, causing apnea and asphyxia.
✅ What is the antidote to curare?
People place more value on the visible muscles of the body, the ones they show off and take pride in.
Few appreciate the invisible muscles that intervene to perform the phases of inspiration (entry of air from the atmosphere into the lungs) and expiration (exit of air from the lungs).
If those muscles responsible for facilitating pulmonary ventilation were to stop working, we would suffocate and die, unless the action is reversed.
Historical documents indicate that the Spaniards tortured the Indians so that they would tell them the antidote for curare, to save themselves from the certain death caused by curare. But no shaman or indigenous healer revealed the traditional knowledge of their people, knowledge that had been passed down from generation to generation and which constituted their heritage and identity.
✅ How did the indigenous people use it?
- For fishing and hunting:
Fishing was facilitated with the help of the barbasco. Hunting, with the help of curare.
- For the war:
In times of war, curare acted as a deadly weapon against enemies.

The indigenous people used curare long before the arrival of the Spanish or Portuguese in the Amazon basin.
They had many ways to elaborate it.
They used different plants to do so, according to the regions where they lived. They developed different blends according to the purposes they pursued. Hence, there is no single type of curare, nor a particular plant, nor a form of mixture.
✅ History of curare
Historically, much was written about the indigenous use of curare, but those reports are filled with inaccuracies.
The first foreigner to describe the use of curare was Pedro Mártir de Anglería (1457-1526), in his book De Orbe Novo. Published 1516, it was later (1493 – 1526) translated as Decades of the New World.
Pedro Mártir never visited America, which is why Bartolomé de las Casas and Fernández de Oviedo doubted the accuracy of his reports. Pedro Mártir wrote that the curare was prepared by a group of old women in secret, who were isolated and often died from inhaling the fumes. That is false. Curare inhaled or consumed orally has no effect.
The Sevillian physician and botanist Nicolás Bautista Monardes (1493-1588) wrote several books. One of them was Historia medicinal de las cosas que se traen de nuestras Indias Occidentales. There he made references to curare and described the ritual of its preparation.
Sir Walter Raleigh
Another reference to curare was made by Sir Walter Raleigh, a privateer in the service of the King of England. Raleigh spent some time in America in search of El Dorado. Returning from the English colony of Guyana in 1595, he recounted his American experience in dramatic tones that were riddled with falsehoods and exaggerations.
He wrote that soldiers wounded by arrows poisoned with curare (also known as ourari), remained immobile, but conscious, staring, and unable to scream or cry during the agony.
In another part of his account he said, in an obvious exaggeration, that sometimes they died in a state of complete insanity, with their intestines protruding from their bellies in a stench that prevented them from being helped or assisted. It was the first description of the muscular paralysis caused by curare, without altering consciousness, which would again be described a few centuries later.
✅ Scientific experiments and other uses.
In 1735 the French Academy of Sciences financed the expedition of a geodesic mission to Ecuador to measure the longitude of the degree of the Earth’s meridian. This mission was led by the French scholar Charles Marie de La Condamine (1701-1774).
After completing his mission south of Ecuador, he made a trip on his own to the Amazon. When he returned to France in 1744 he published a book in which he made reference to the rubber and cinchona plants, noting that he obtained samples of curare paste with which he conducted some experiments using chickens.
Brockelsby
In those years, curare was studied at the University of Leiden, in the Netherlands. The Englishman Brockelsby reported experimenting with curare by injecting it into a cat’s paw. He observed that the animal’s breathing failed, while its heart continued to beat for more than two hours.
Fontana
In 1780, the Florentine abbot Felix Fontana, also from the University of Leiden, recorded that curare was harmless when taken orally and that its inhalation did not cause poisoning.
Humboldt
Alexander von Humboldt (1769-1859) explored Venezuelan territory between 1799 and 1804. Later, in his book Diario de viaje a las regiones equinocciales del Nuevo Continente, he recounted in detail the process of producing curare in the Upper Orinoco, noting that it was poisonous in the blood, but that it was used orally as a medicine.
Waterton
In 1812 Charles Waterton, an English naturalist and taxidermist, traveled to British Guiana and took curare specimens to London. In an experiment he injected curare into the leg of a donkey, but first he had tied it tightly to block the passage of the poison.
After the injection, the donkey walked without problems. He then removed the ligature, and ten minutes later the animal collapsed and died of asphyxiation.
Brodie
That same year, surgeon Benjamin Brodie, a member of the Royal Society in London, performed a test on a donkey, without ligating its limb. In a few minutes, the animal became paralyzed, its breathing stopped, while its heart continued to beat.
He then immediately performed a tracheotomy and managed to resuscitate the animal, maintaining rhythmic ventilation for two hours. Then the animal sat up. He survived, and managed to live two more years after the experiment. Brodie also demonstrated that curare killed by asphyxiation, without causing great effects on the heart or brain.
✅ The various types of curare
It had not been noticed that the curare used in the different tests was not the same.
The one from British Guyana and the Orinoco River basin was made from the bark and roots of a vine of the strychnos genus and contained strychnine, with predominantly convulsant effects, which masked the paralyzing effect of curare.

The other samples came from the Ecuadorian and Peruvian Amazon and were prepared using as a base another vine, Chondrodendron tomentosum, with a high curare content.
✅ How is curare prepared?
Alexander von Humboldt made one of the first descriptions of the preparation of curare paste. He had seen it prepared in the Upper Orinoco on his trip to Venezuela, between 1799 and 1804.
Another description has been attributed to Richard Evans Schultes, an explorer and botanist who has been considered the father of ethnobotany. He lived for some years in the Putumayo region of the Colombian Amazon and saw many times its preparation among the cofanes (Schultes 1991: 265).
Curare is prepared by a shaman, who learned the technique from another shaman, passing the knowledge from one generation to the next. Before preparing the substance, which ends up being a dense black paste, the shaman would fast. Curare is usually a mixture of several plants of the genera Chondrodendon and Strycnos.
Schultes said that there are compounds that have up to 15 ingredients, although there are also single-species compounds.Some of the added elements may not be toxic, but serve as accelerators of the process, as is the case of Ocotea venosa, Unonopsis veneficiorum, or species of the genus Capsicum .
✅ Claude Bernard changes the medical perspective.
In Paris, in 1845, the French scientist Claude Bernard (1813-1858) received the Physiology Prize from the Paris Academy of Sciences for his research on curare.

His medical observations, presented in the form of lectures in his book Lecons sur les effects des substances toxiques et medicamenteuses, were published in 1856.
From lesson 16 onwards, he discussed curare, which according to his biographer Oriol Martí (2006:64), is “the substance that most helped him to build his pharmacological thinking”.
Lesson 16 begins with a historical study on the origin of curare and discusses the preparation techniques and its uses among the ethnic groups of the region. The lesson also reviews the geographical discoveries and the trips of naturalists to the Amazon and Orinoco basin.
Lesson 17 studies the physical and chemical properties of curare.
Lesson 18 then considers the physiological actions of curare and its absorption forms on mucosal surfaces.In lesson 19 he explains in detail his pharmacological experiences with curare and its effects on mammals, reptiles and birds.
On the other hand, in the following lessons Bernard describes the transient effects of curare, warning that it does not create an anatomical lesion on the tissue, “because it is not necessarily morphological, and once it disappears, the function is normalized”.
Lesson 23 shows that curare acts selectively on the motor nervous system, which can be destroyed without the muscles losing the faculty of contractility.
And finally, in Lesson 24, he compares curare with other substances that are characterized by causing paralysis.
Bernard discovered that curare acts on the neuroeffector junction of skeletal muscle by blocking its stimulation of the nerve impulse.
His experiments conducted between 1844 and 1856 were carried out with curare samples obtained in Brazil by one of his laboratory colleagues.
Let us remember that we are in Paris in 1856. It was not known what was a neurotransmitter, nor had acetylcholine been isolated. Experiments in neuroscience were just beginning, and not much was known about neurons.
Bernard explained how curare blocked neuromuscular transmission, interrupting the transmission of electrical impulses from nerves to muscles.
Experimenting with frogs, he showed that curare acted selectively by blocking messages to the motor nerves reaching the muscles. Alfred Vulpian, a disciple of Bernard’s, observed that curare applied near the motor plate or the site of neuromuscular attachment acted rapidly. But it was not clear why.
Eighty years later things began to become clearer.
✅ Acetylcholine, the missing piece of the puzzle.
In 1935, Dr. Harold King, of the National Institute for Medical Research in London, isolated a crystalline substance from a sample of curare provided by the British Museum. That sample was contained in a unique container: a reed or tube made from a section of bamboo. It was labeled “Ucayali River 1871”. King called it d-tubocurarine.
Acetylcholine. Source: Yohan [Public domain]
Neurotransmission, then, was only a hypothesis.
The physiologist Henry Dale had discovered acetylcholine in 1910. His friend Otto Loewi, who lived in Austria, had discovered in his experiments with frogs that neurotransmission occurred in the autonomic nervous system, but the neurotransmitter was unknown.
Dale speculated that it might be acetylcholine, and Loewi proved that to be true.
Acetylcholine was the neurotransmitter. For this discovery Dale and Loewi received the 1936 Nobel Prize in Medicine.
That discovery that a chemical substance, acetylcholine, acted as a neurotransmitter proved that the nerve impulse was transmitted chemically and not electrically.
Acetylcholine receptors. Source: Burns et al, 2012 [CC BY-SA 4.0 (https://creativecommons.org/licenses/by-sa/4.0)]
It was then known with certainty that curare blocked the action of acetylcholine in a particularly sensitive area of the muscle, and that the muscle contraction necessary to activate the muscle did not occur. This resulted in progressive paralysis of the muscles. Year later, Neher and Sackman, physiologists at the Max Planck Institute in Germany, demonstrated how chemical neurotransmitters work at the molecular level and how their action was blocked by curare.
✅ Medical use of curare (serendipity).
Richard Gill was a director of a company that exploited rubber in the Ecuadorian Amazon.
While riding a horse, he had an accident and was left semi-paralyzed, suffering from spastic paresis.
He returned to the United States to recover with therapies, but suffered from intense pain in the extremities on the right side of his body. He thought that the curare used by the indigenous people of the area to relieve muscle pain could help him.
He traveled to Ecuador in 1938, bringing back with him some thirteen kilos of prepared curare, to have it purified and clinically tested in the United States.
This curare, made from various types of liana, was delivered to the E.R. Squibb Laboratories where it was purified under the trade name of Incostrin and given to researchers seeking clinical uses for the product.
It was already known that the raw material of curare came from two types of plants: menispermaceae, such as Chondrodendron tomentosum, and logoniaceae(Strychnos toxifera), and that the active ingredient of curare was d-tubocurarine.
Serendipity is a fortunate outcome, which occurs by chance or accident without being sought after. This was the case, for example, with penicillin, but also with curare.
Intocostrin
Intocostrin came into the hands of a Nebraska psychiatrist named Bennet, who used it to reduce seizures associated with the administration of a drug as an alternative to the application of the electro-shock technique.
It was also used to treat spastic children.
It was also given to Lewis Wright, a New York hospital anesthesiologist who incorporated it into his practice in 1940. He contacted a friend, Dr. H.R. Griffith, head of the anesthesiology department of the Homeopathic Hospital in Montreal, Canada. Dr Griffith used cyclopropane instead of ether, which enhances the effectiveness of the anesthesia. He successfully applied it many times, and published his results in the American Journal of Anesthesiology in 1912.
Griffith demonstrated, through his continued medical practice, that d-tubocurarine was a safe muscle relaxant in surgical procedures.
Tubocurarine
Thus began the use of tubocurarine in anesthesiology. Earlier, in 1912, it had been used by surgeon Arthur Lawen, in Leipzig, but the results were ignored and its use was interrupted due to lack of curare supplies (Bustamante 2017).
With Daniel Bovet’s (1907-1992) discovery of galamine around 1946, the use of curare in anesthesiology began to decrease. Galamine proved to be a much safer muscle relaxant for use with anesthetia.
Two years later, in 1949, Bovet synthesized succinylcholine, which was much safer and faster as a muscle relaxant. Succinylcholine began to be widely used as a muscle relaxant in 1951. For this discovery he was awarded the Nobel Prize in Medicine in 1957.
Curare continued, however, to be applied in medical practice in the treatment of diseases that cause convulsions. In Peru and Brazil it is also used to treat excessive menstrual bleeding and to relieve bruises.
✅ Bibliography
- Bustamante B, R. (2017). History of neuromuscular blockers. Chilean Journal of Anesthesiology. 46: 116-130.
- Dale H.H., Fedberg W, Vogt M. (1936). Release of acetylcholine at voluntary motor nerve ending. Journal of Physiology, 86: 353-380.
- Feldman S. (2009). From poison arrows to Prozac. London: John Blake Publishing.
- Gill R.C. (1940). White Water and Black Magic. New York: Henry Holy & Co.
- Griffith H.R., Johnson G.E. (1942). The use of Curare in general anesthesia. Anesthesiology, 3-4, 418-420.
- Humboldt A. (1998). Wonders and mysteries of Venezuela. Journal of travels to the equinoctial regions of the New Continent. Caracas: Ediciones CEC.
- King H. (1935). Curare Alkaloids: Curarine tube. Journal Chem. Soc. 1381-1389.
- López Tricas J.M. 2017. History of curare. INFO-Pharmacy.com. Zaragoza.
- Martín Barbero M.L. and Guijarro M. (2011-2012). Pharmacologic interactions of drugs used in anesthesia, 404-431. Girona Brumós L. Introduction to drug interactions . Madrid: CSEFH- Curso de Interacciones.
- Martí O. (2006). Claude Bernard and experimental medicine. Spain, Montesinos: Ediciones de Intervención Cultural.
- Padfield A. (2017). Charles Waterton (1782- 1865) and Wourali. Archives of Natural History, Vol. 44, No. 1, 122-129.
- Piojan M (2007). Lethal poisons. Pharmaceutical field. Ethnopharmacy. Q. Farm. Vol. 26, No. 4, 104-116.
- Raleigh W. (1820). Brief and admirable description of the Kingdom of Guyana. Edinburgh.
- Repetto-Jiménez M, Repetto Kuhn G. 2001. Fundamental toxicology. Bruneton J. Pharmacognosy, phytochemistry, medicinal plants. Mexico: Ediciones Acribia.
- Resiszienzia.18.10. 2014. Curare: what matters is not the poison itself, but how it is used. Scirescience.wordpress.com/2014/04/18/cure-what-imppirta-is-not-venom-no-how-to-use.
- Schultes R.E., Hofmann A. (1979). Plants of the Gods: origins of the use of hallucinogens. Mexico: Fondo de Cultura Económica.
- Steinberg D; Chalita J. (2000). Fascinating versions and controversies about curare. Muscle relaxants. Alvarez J.A., Gonzalez F., Bustamante R. Anesthesia and Intensive Care. Madrid: Aran Ediciones.
Author

Dr. Rafael Cartay is a Venezuelan economist, historian, and writer best known for his extensive work in gastronomy, and has received the National Nutrition Award, Gourmand World Cookbook Award, Best Kitchen Dictionary, and The Great Gold Fork. He began his research on the Amazon in 2014 and lived in Iquitos during 2015, where he wrote The Peruvian Amazon Table (2016), the Dictionary of Food and Cuisine of the Amazon Basin (2020), and the online portal delAmazonas.com, of which he is co-founder and main writer. Books by Rafael Cartay can be found on Amazon.com
Proofreader
Related Posts
May 15, 2020

Amazon Rainforest DANGEROUS Animals (TOP 10)
January 16, 2020

4. Great naturalist scientists in the Amazon Rainforest (18th to 19th centuries)
November 17, 2019

Cane Toad / Giant Toad (Rhinella marina)
November 17, 2019

Kambo (Phyllomedusa bicolor)
October 19, 2019
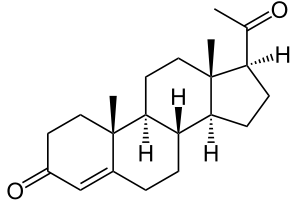
Barbasco: What is it for? Poison and medicine + 10 species
October 5, 2019
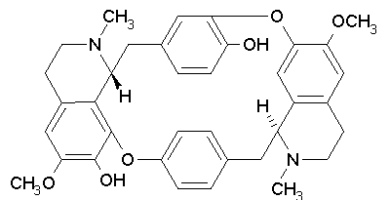
Amazon Rainforest Poisonous Plants
This post is also available in:
![]() Español (Spanish)
Español (Spanish)
